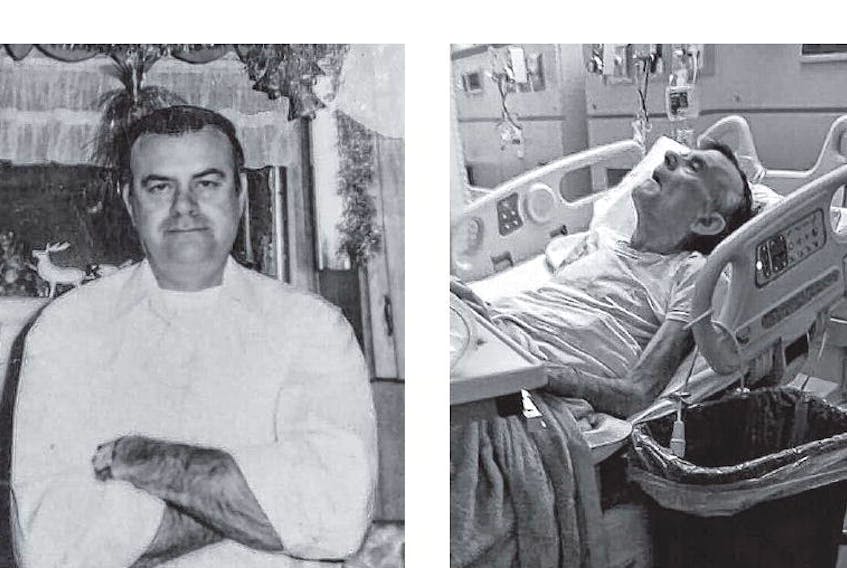
Denton Brown spent two days dying on a stretcher beside the utility closet in the Cumberland Regional Health Care Centre’s emergency room.
His daughter, son and sister stayed with him in shifts at the hospital in Upper Nappan, near Amherst, because there wasn’t room for all of them to be with him at once.
“My father, who worked hard all his life, spent his final two days beside the dirty utility room with visitors, staff and patients going by, staring at him while he struggled to breathe,” said Margaret Brown, Denton’s daughter.
“I don’t mean to harp on it, but they brought him brown-bag meals with a wet old turkey sandwich. He deserved better than this.”
While the Brown family is speaking out, they are not the only ones to have gone through the death of a loved one in the midst of the swirl of activity in a hallway in a busy Cumberland County emergency room.
“You have no idea how many times we’ve had to try to find a place for someone in a hallway to let them die with dignity,” said Dr. Brian Ferguson, an Amherst family physician who also works in the emergency room.
Denton Brown’s experience with end-of-life care began three months before his Jan. 22 death.
Each step of his encounter with the health-care system during those months paints the picture of an infrastructure struggling to cope with the growing needs of an aging population.
Denton may have died poorly but he lived well.
Life was all outside for the Brown family of South Brook Road. They have lived on the same 40 hectares since the mid-1800s and still have their own family cemetery across from the homestead. Denton grew up working with his father in their sugar woods. At 21 he had already developed a lifelong love affair with heavy machinery when he married Linda Slack.
“Anything we wanted, he’d do his best to get it for us,” said Jamie Brown. “He worked all the time and was a quiet, private man.”
Denton operated his own dump trucks and logging skidders, and then in his mid-40s started driving snowplows for the Transportation Department. Linda worked as a cook’s aid at High-Crest Nursing Home in Springhill, and together they maintained blueberry fields, kept a big vegetable garden and went to local dances.
Their health started to fail quickly upon their retirement at 65.
Linda began forgetting things and Denton, who had smoked up until his early 60s, suffered from COPD.
“I know what people will say, that he brought it on himself by smoking,” Margaret said.
“He grew up in a generation that glamourized smoking and, by the time he knew it was bad for him, he was addicted. You drive a snowplow around Lower Cove in a blizzard and tell me you wouldn’t want a cigarette.”
Jamie and Margaret stepped in. For the next four years they cooked, cleaned and paid bills for their parents. But by last spring Linda was forgetting to eat and Denton was spending days sleeping in his chair.
In July, their family doctor made a home visit.
“He told us dad was terminal and that they couldn’t be in that house for another winter,” said Margaret.
Two days before their assessment for long-term care residency, Denton was rushed to the emergency room. He weighed 99 pounds and had critically low oxygen in his bloodstream.
“They put him on an IV and gave him oxygen and, after a chest X-ray, the doctor told us Dad’s lungs were done,” said Margaret.
But despite his deteriorating condition and the warning from their family doctor, Denton was assessed to not qualify for palliative care.
There are no dedicated palliative care beds in Cumberland County.
Denton also didn’t qualify for a residential care facility.
“They said it was because he was still eating and could walk and had his mind,” Margaret said.
The Nova Scotia Health Authority declined to comment on the specifics of Denton’s case, citing patient confidentiality. But the authority did confirm that it has a home-first policy.
Cheryl Northcott, the authority’s executive director of operations, said most patients prefer to age in their homes and that nursing and personal care support is provided through the Victorian Order of Nurses.
If residents can’t safely stay in their homes, there are two types of facilities available to them.
Nursing homes offer a higher level of care where there is 24-hour nurse supervision and residents can get assistance with every aspect of daily life.
Residential care facilities do not have 24-hour nurse supervision, but care workers can assist residents with self-care like bathing and dressing.
Linda was assessed to require a nursing home and was put on a waiting list.
Margaret took a leave of absence from her job as a continuing care assistant with the VON so she could care for her mother full time.
Meanwhile, she and Jamie hired a lawyer and appealed the assessment of their father as not qualified for a long-term care facility. The decision was reversed and Denton was sent to White Birches in Amherst and Linda to a higherlevel care home in Pugwash just after Christmas.
“I think separating them killed him,” said Margaret.
“They’d been married for almost 50 years and didn’t want to be apart.”
According to the health authority, Cumberland County has a higher percentage of residents over age 65 than any other county in Nova Scotia.
That, said Northcott, means a greater demand on the entire health-care system than in areas with a younger population.
Denton and Linda were on a list to be reunited but on Jan. 18 Margaret got a call from staff at White Birches. Denton was seeing tractors and snowplows coming down the hallway of White Birches and was struggling to breathe.
On the morning of Saturday, Jan. 20, having been diagnosed with pneumonia, Denton was taken to the emergency room of the Cumberland Regional Health Care Centre.
He was put on an IV and given antibiotics but remained until Sunday evening on a stretcher in the hallway next to the utility room.
“Sometimes you go and no one is waiting in the emergency room, other days you go down and it’s full,” Northcott said.
“The nature of the business is that there are peaks and valleys of activity. There are occasions when we have had patients on stretchers in the hallway.”
Northcott said she wasn’t in a position on Friday to state whether the regional hospital is operating beyond its capacity.
Dr. Ferguson, however, was.
“We built our emergency room too small — it can’t be a regional hospital for 34,000 people and only have 11 beds (in the emergency room),” said Ferguson, who has worked as a doctor in Amherst for 31 years.
One thing both Northcott and Ferguson agree on is that the health-care system is a flow, with people constantly being admitted and discharged.
If at some point in that system a backlog is created, every step of the system before it begins backing up.
Of the hospital’s 72 beds, only four are currently occupied by people waiting placement in a long-term care home. However, 16 people have been medically discharged but can’t yet return home for a variety of reasons, ranging from renovations to accommodating their mobility issues to waiting for additional supports to be put in place.
“Overcrowding in the emergency department is a symptom of the challenges we have in getting patients admitted on a timely basis and, on the other end, trying to discharge patients elsewhere,” Northcott said.
Because all the hospital beds are sometimes occupied, there are seven stretchers in the emergency room that are considered beds and have curtains that can be wrapped around them for privacy.
Denton didn’t get a stretcher with a curtain, despite Margaret asking for one.
While the family sat with Denton in shifts, Margaret said she overheard a doctor ask a nurse Saturday night, “How many emergency rooms are closed tonight?”
Beyond backlogs, the system can get flooded by too many patients.
Four smaller hospitals in Tatmagouche, Pugwash, Parrsboro and Springhill have all had repeated emergency room closures due to a shortage of doctors. In October, the smaller emergency rooms were closed 50 per cent of the time.
Bruce Saunders, chairman of the former Cumberland Regional Health Authority, said when people don’t know if their local emergency room is open, they often then go to the regional hospital.
“My impression is that with the repeated closures (of the smaller hospitals), the public confidence is again lost,” said Saunders.
For his part, Ferguson said the regional hospital’s emergency room was not designed to handle patients coming from all over the county.
“I sat on the committee that designed that emergency room and at the time lobbied for some of the smaller emergency rooms to be closed so that we could have a larger one,” Ferguson said. “I was told that would be political suicide.”
And now, said Ferguson, those smaller emergency rooms end up being essentially closed by default.
Combine that with what he estimates to be a shortage of 100 residential care and nursing home beds in the county, said Ferguson, and you have patients who die on stretchers in the hallway.
“We have an aging population and we can’t recruit doctors — we are headed for an Armageddon,” said Ferguson. “The problem will get worse.”
Meanwhile, Jamie and Margaret just wanted a bit of privacy to be with their father while he died.
On the evening of Sunday, Jan. 21, Denton was rolled into a room with five other patients — all in their own distress.
He died at about 1:30 a.m. with his children and siblings by his side.
He was 71 years old.
Linda’s dementia has progressed and Margaret has explained to her twice that the man she loved for 50 years is dead.
“We’re not telling her any more,” said Margaret.
“She doesn’t have to worry about dying any more.”
Though Margaret received an apology from a staff member at the hospital, what she wants is for no one else to have to die like her father did.